Mayo Foundation (more.)Ī distinctive pattern, which may be seen in some encephalopathic or even comatose patients, is lateralized periodic discharges (LPDs, formerly known as PLEDS), which may be focal, unilateral hemispheric, or even bilateral and independent. Waveforms show characteristic anterior to posterior lag (see waveform marked by black arrow). Generalized triphasic wave pattern and slowing in a 72-year-old man with hepatic encephalopathy. EEG in a delirious patient may show either diffuse nonspecific nonepileptiform background slowing, or even epileptiform-appearing patterns such as triphasic waveforms (see Figure 56 for triphasic wave pattern), which are most common in patients with underlying associated hepatic or renal impairment or both, and resultant encephalopathy, although similar patterns may be induced by drug intoxication or adverse effects or other nonlesional causes of severe generalized cerebral dysfunction. Encephalopathic patients may have acute symptomatic seizures, resulting in diagnostic confusion. The clinical phenomena of confusion in a delirious state may closely resemble a complex partial or atypical absence seizure, involving blank staring with disorientation, inattention, and variable responsiveness, stupor with reduced vigilance, and unusual movements including myoclonic jerks. Specific examples of clinical phenomena associated with generalized slowing on the EEG are discussed below.ĭelirium, also known as encephalopathy, is a reversible generalized confusional state induced by a systemic disorder. See Figure 55 for an example of generalized EEG slowing resulting from a metabolic encephalopathy. Several different etiologies may provoke generalized background slowing, including the effects of sedative centrally acting medications, neurodegenerative disorders, a widespread neurodevelopmental process, hydrocephalus, metabolic or toxic encephalopathy, CNS infectious disorders such as meningoencephalitis, or even a focal midline structural lesion involving deep midline brainstem, diencephalic structures, or both (producing a phenomenon known in older EEG literature as a “distance or projected rhythm,” which often selectively involves the anterior or bifrontal areas and produces a pattern known as frontal intermittent rhythmic delta activity, or FIRDA).
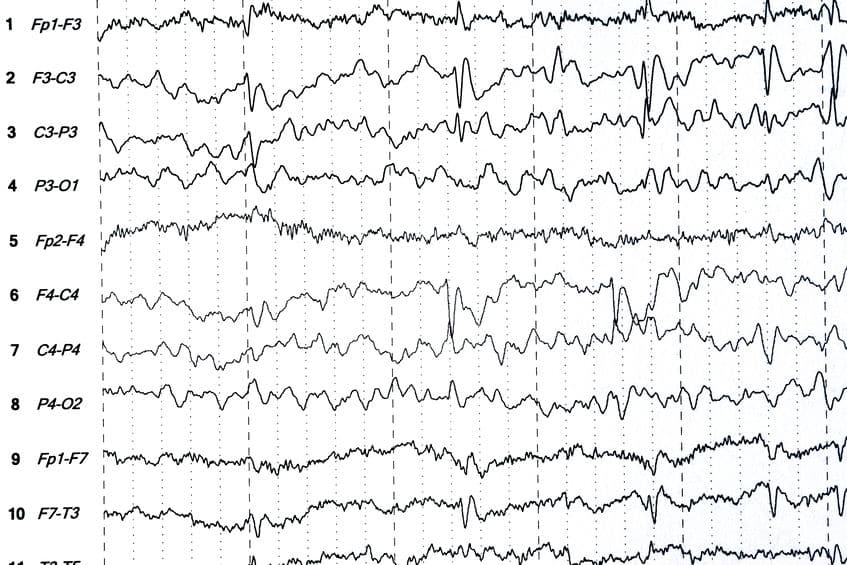
Generalized background slowing indicates diffuse cerebral dysfunction, which, similar to focal slowing, is also not specific as to cause. See Figure 54 for an example of focal temporal regional slowing, which also shows a “breach rhythm,” with focally elevated background amplitude as a result of a skull defect and previous surgery in this area.

The various causes are too numerous to be comprehensive, but common examples include transient or permanent ischemia resulting from stroke, brain hemorrhage, tumors, traumatic injury, malformations of cortical development, nonstructural focal cerebral dysfunction corresponding to a focal epileptic focus, focal involvement of the cortex by neurodegeneration, arteriovenous malformations, and focal brain infection caused by bacterial cerebritis or viral encephalitis. Focal brain lesions of a variety of causes to cortex, underlying white matter, or both may induce focal slowing. When intermittent, focal slowing may indicate unveiling of subtle focal cerebral dysfunction owing to the effects of a sedating or hypnotic medication, although usually medication-induced slowing is generalized in nature. A variety of etiologies for focal cerebral dysfunction may be seen.
Slowing may be intermittent or persistent, with more persistent or consistently slower activity generally indicating more severe underlying focal cerebral dysfunction.

Focal slow wave activity on the EEG is indicative of focal cerebral pathology of the underlying brain region.
